Home » Can You Breastfeed After Breast Augmentation Surgery?
Can You Breastfeed After Breast Augmentation Surgery?
Posted by Dr. David W. Allison

Many women considering breast augmentation wonder whether they will be able to breastfeed in the future. Others already have breast implants and want to understand how their prior breast surgery may affect nursing. This is a common concern for mothers planning to grow their families while also pursuing cosmetic surgery.
The ability to breastfeed after augmentation mammoplasty depends on several factors, including implant placement, incision technique, preservation of breast ducts and nerves, and individual healing. With careful surgical planning and proper support after delivery, many women with breast implants are able to produce human milk and successfully nurse their infants.
Key Facts About Breastfeeding After Breast Augmentation
Breast augmentation and breastfeeding are closely connected topics for many patients. Understanding how surgery may affect nursing helps women make informed decisions about treatment and family planning.
- Most women with breast implants can breastfeed successfully.
- Surgical factors such as implant placement and incision type matter.
- Milk supply varies based on preserved glandular tissue and nerve function.
- Breast implants are generally considered compatible with breastfeeding.
- Planning ahead with an experienced plastic surgeon supports better outcomes.
Can You Breastfeed After Breast Augmentation?
Yes, many women with implants are able to breastfeed and provide enough breast milk for their children. However, results vary depending on the type of surgery performed and how the body heals afterward.
Breast augmentation does not automatically prevent nursing. The procedure typically focuses on enhancing breast size while preserving milk-producing structures whenever possible. When breast ducts, nerves, and glandular tissue remain intact, milk production and milk flow can occur normally.
Some mothers may experience reduced supply or require supplementation, but exclusive breastfeeding is still possible for many women with implants. It is also important to note that variations in milk supply can occur in women without breast implants.
How Breast Augmentation Surgery Can Affect Breastfeeding
Breast augmentation changes the structure of the breast, which can influence milk production or delivery in certain cases. The impact of breast implants depends on how surgery interacts with breast tissue and nerves involved in nursing.
Impact on Breast Ducts
Breast ducts carry milk from glandular tissue to the nipple. If ducts are disrupted during breast surgery, milk flow may be reduced.
Modern augmentation mammoplasty techniques aim to preserve these structures. However, surgical approaches that involve the nipple area may increase the likelihood of affecting milk pathways.
Impact on Nerves Involved in Milk Let-Down
Nerve function plays a major role in breastfeeding. Sensation in the nipple triggers hormonal signals that stimulate milk production and release.
If nerve pathways are altered, mothers may experience difficulty with the let-down reflex. In many cases, nerve function improves over time as healing progresses.
Impact on Breast Tissue and Glands
Glandular tissue produces milk. During cosmetic surgery, surgeons work to protect this tissue whenever possible.
Some patients, particularly those with hypoplastic breasts or limited glandular tissue before surgery, may already have reduced milk-producing capacity regardless of augmentation.
Changes in Milk Production After Surgery
Women with implants may experience different outcomes, including:
- Full milk supply and successful nursing
- Partial supply with supplementation
- Minimal milk production due to surgical or anatomical factors
Each case varies based on the type of surgery and individual healing.
Does Implant Placement Affect Breastfeeding Success?
Implant placement is an important surgical factor that can influence breastfeeding outcomes.
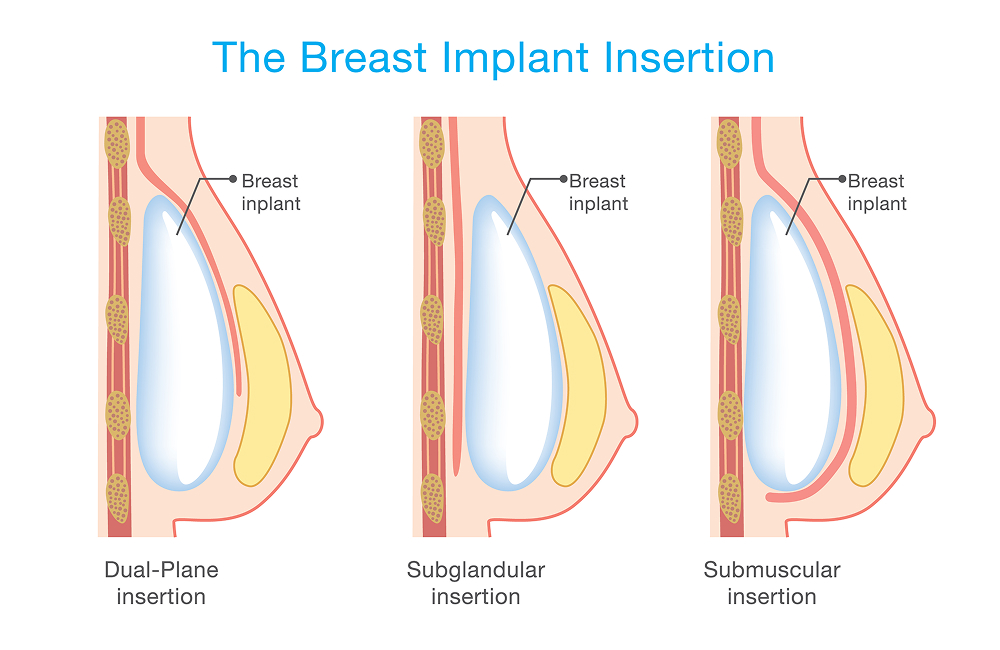
Over-the-Muscle Implant Placement
Subglandular placement positions the implant above the chest muscle and beneath breast tissue. This approach may place more pressure on milk glands, which could affect milk production in some patients.
Under-the-Muscle Implant Placement
Submuscular placement positions the implant beneath the chest muscle. This technique typically has less direct contact with glandular tissue and may reduce interference with milk production.
Many plastic surgeons consider this approach when patients plan future pregnancies.
Dual-Plane Implant Placement
Dual-plane implant placement combines elements of both approaches. The implant sits partially beneath muscle and partially beneath breast tissue, allowing natural contouring while supporting preservation of milk-producing structures.
How Incision Location Affects Nursing After Breast Surgery
The location of the surgical incision can influence the impact of breast implants on breastfeeding ability. Different approaches carry varying levels of risk for affecting breast ducts or nerves.
Periareolar Incision
This incision follows the edge of the areola. Because it is close to milk ducts and nerve pathways, it may increase the risk of disruption in some cases.
Inframammary Incision
An incision placed beneath the breast fold typically avoids direct contact with glandular tissue and ducts. This approach is commonly used and generally has minimal impact on nursing.
Transaxillary Incision
This technique places the incision in the armpit. Because it avoids direct breast tissue disruption, it usually preserves structures involved in breastfeeding.

TRUSTED, EXPERT CARE FOCUSED ON PRECISION AND CONFIDENCE
Dr. Allison provides patients throughout NJ and PA with expert care designed to deliver refined, natural-looking results.
Are Silicone Breast Implants Safe for Breastfeeding Babies?
Safety is a frequent concern among mothers with implants. Current research on breastfeeding and silicone breast implants is limited, but available evidence has not shown recent reports of clinical problems in infants of mothers with silicone implants. Major medical organizations state there is insufficient evidence to consider silicone breast implants a contraindication to breastfeeding.
Breastfeeding provides significant benefits for infants, and women with silicone breast implants or saline implants are typically encouraged to nurse if they are able. Patients with specific concerns should discuss their situation with their physician.
Signs You May Be Able to Breastfeed Successfully After Augmentation
Certain indicators suggest that breastfeeding may be possible following augmentation mammoplasty.
Preserved Nipple Sensation
Normal sensation suggests intact nerve pathways involved in milk release. Sensation may be temporarily altered after breast surgery but often improves as healing continues.
Breast Changes During Pregnancy
Breast enlargement, tenderness, and fullness during pregnancy indicate active glandular tissue.
Milk Production After Delivery
The ability to produce colostrum or experience breast fullness after birth often signals functional milk production.
Challenges Some Mothers May Experience
Although many women with implants can nurse successfully, some may encounter challenges related to milk supply or delivery.
Insufficient Milk Production
Some mothers may not produce enough breast milk due to surgical factors or limited glandular tissue.
Delayed Milk Production
Milk may take longer to come in after delivery, requiring close monitoring.
Difficulty With Let-Down Reflex
Nerve changes may affect hormonal signaling involved in milk release.
Breast Pressure or Engorgement
Implants may contribute to feelings of fullness or pressure that require careful management.
Tips to Improve Breastfeeding Success After Breast Augmentation
Women with breast implants can often improve nursing outcomes through proactive care and support. These steps help stimulate milk production and support infant nutrition.
- Begin nursing soon after delivery to stimulate milk production.
- Breastfeed frequently to encourage ongoing milk removal.
- Work with a lactation consultant for guidance and technique adjustments.
- Monitor infant weight gain to ensure adequate nutrition.
- Use pumping when needed to increase milk supply.
- Maintain hydration and balanced nutrition.
Early support can help mothers establish consistent milk production and address challenges quickly.
When to Talk to a Plastic Surgeon or Doctor
Open communication with healthcare providers helps women prepare for breastfeeding and manage concerns related to breast surgery.
Before Breast Augmentation
Women planning future pregnancies should discuss surgical options and implant placement with their plastic surgeon.
During Pregnancy
Monitoring breast changes helps assess potential milk production.
After Delivery
Persistent low supply or nursing difficulty should be evaluated promptly.
Breast Augmentation vs Breast Reduction or Breast Lift and Breastfeeding
Different types of breast surgery affect breastfeeding in different ways.
Breast augmentation typically focuses on enhancing size while preserving existing tissue. Breast reduction and reconstructive surgery procedures may remove glandular tissue, which can more directly affect milk production. Breast lift procedures may also influence nerve pathways depending on technique.
Understanding the type of surgery performed helps patients anticipate potential outcomes.

About Dr. David W. Allison
Dr. David W. Allison is a board-certified plastic surgeon providing cosmetic and reconstructive surgery of the breast and body. With more than 21 years of surgical experience, he offers breast augmentation procedures tailored to each patient’s anatomy, goals, and long-term health considerations.
He emphasizes careful surgical planning, patient education, and individualized treatment strategies designed to support both aesthetic results and functional outcomes. Patients receive comprehensive guidance throughout the consultation process to help them make informed decisions about breast surgery.
Schedule a Consultation
Women considering breast augmentation or concerned about the impact of breast implants on future breastfeeding can benefit from personalized guidance. A consultation provides an opportunity to discuss surgical options, implant placement, and long-term goals such as nursing and family planning.
Dr. Allison evaluates each patient’s anatomy, health history, and treatment priorities to recommend the most appropriate approach. Contact the practice to schedule an appointment and learn more about breast augmentation options.
Frequently Asked Questions
Can women with silicone breast implants produce enough breast milk?
Many women with silicone breast implants are able to produce enough breast milk for their infants. Milk supply depends on preserved glandular tissue, nerve function, and individual healing.
Does implant placement affect breastfeeding outcomes?
Yes. Implant placement may influence how much pressure is placed on glandular tissue. Under-the-muscle placement typically has less direct interaction with milk-producing structures.
Are breast implants safe for infants?
Current research is limited, but available evidence has not shown recent clinical problems in infants of mothers with breast implants. Breastfeeding is generally encouraged when possible.
Can breast surgery cause insufficient milk production?
Some surgical techniques may affect milk supply if breast ducts, nerves, or glandular tissue are disrupted. Many women still produce partial or full supply.
Should mothers with implants work with a lactation consultant?
Yes. Lactation support can help address challenges, improve milk production, and ensure infants receive adequate nutrition.
Breastfeeding After Breast Augmentation Is Often Possible
Most women with breast implants can breastfeed successfully. Surgical technique, implant placement, and preservation of breast tissue play important roles in determining outcomes. Professional support from a plastic surgeon and lactation specialist can help mothers address challenges and improve breastfeeding success.
Women considering augmentation mammoplasty should discuss future pregnancy plans and nursing goals with an experienced plastic surgeon to support both aesthetic and functional results.
